As the healthcare landscape continually evolves, the significance of Star ratings has never been more pronounced.
In the 2020 Star Ratings, member experience measures constituted only 31% of the total weight. This proportion is set to increase to 58% in the 2023 Star Ratings. For payor organizations, this challenging landscape requires a vastly improved member experience to differentiate themselves — every time.
Member and patient experiences are now a top priority.
As the Centers for Medicare & Medicaid Services shifts its focus, weighting member experience more heavily in the Star ratings, the urgency for payor organizations to prioritize and enhance quality improvement is paramount.
Traditional Stars Analytics Stop Short of What Business Need to Act
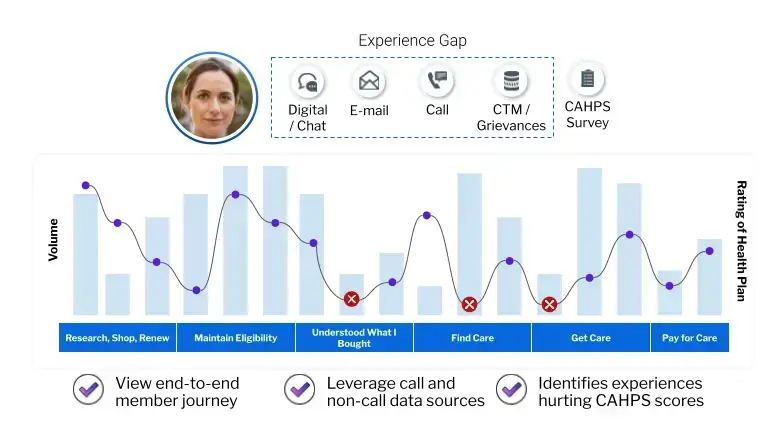
A traditional approach to Stars improvement is no longer sufficient. The key to success lies in effectively identifying and prioritizing actionable insights throughout each and every segment of the member journey before official CAHPS surveys. Now, more than ever, an early warning system that leverages data across all channels of member experience is crucial to the bottom line.
The Time for Change is Now
Qualtrics enables payor organizations to understand the "why" behind CAHPS scores, proactively pinpointing issues that most significantly impact member experience along key journeys, and drive meaningful action. Organizations can easily unite their simulation CAHPS and other member data across different interactions like surveys, calls, chats, or the Complaints Tracking Module (CTM).
Unifying these sources and data clarifies what experiences are truly holding back specific CAHPS scores metrics, allowing the organization to act on systematic issues. One client was able to analyze more than 20 million feedback records, isolate contract-specific CAHPS drivers for poor performance, and implement a remediation process targeted at specific members and regions to drive improved CAHPS scores.
A Modern Approach, A Superior Experience
In the digital age, relying only on Official and Simulation CAHPS data is no longer enough to meet the needs of a rapidly changing Stars landscape. By harnessing a more modern approach, organizations can gain real-time insights to drive higher CAHPS scores.
This means developing member profiles that encompass not just member experience history, but segmentation data as well. This allows organization to identify priority segments that require proactive outreach to drive improved CAHPS scores. And this is all done with one platform serving as a unified source of truth for both regulatory and non-regulatory programs, optimizing the total cost of ownership.
Substantial Success Stories
Our customers have seen tangible results from taking a modern approach to Stars. These results include:
- $75M increase in quality bonus payments due to improving Star ratings by half a star
- Increased Overall Health Plan Rating score by 4 points (on a 100-point) scale solely through target service recovery
- Proactive intervention with key member segments having difficulty ‘Getting Needed Care’
Why Qualtrics and Farlinium
Qualtrics provides the purpose-built, industry-specific solution, and Farlinium contributes deep consulting expertise in setting up and maximizing the value from the solution. Our dedicated team, equipped with vast experience in CAHPS payor programs, ensures that customers not only implement the solution, but also derive the maximum value from it.
With our combined strengths, we cover a range of regulatory programs including HEDIS, QHP, and MA PDP. Our intuitive dashboards facilitate seamless engagement with members through web, mail, and phone, all the while ensuring top-level security with HIPAA, HITRUST, GDPR, and FedRAMP compliance.
Modernize your Stars program with Qualtrics + Farlinium



